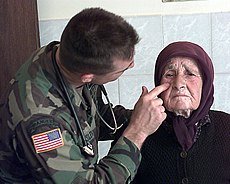
 US Army physician assistant, checks the face of an elderly Serbian womanA physician assistant or physician associate(PA) is a health care practitioner who practices medicine in collaboration with or under the (indirect) supervision of a physician, depending on state laws (equivalent to a nurse practitioner). Physicians do not need to be on-site with PAs and collaboration or supervision often occurs via electronic means when consults are necessary. Their scope of practice varies by jurisdiction and healthcare setting.
US Army physician assistant, checks the face of an elderly Serbian womanA physician assistant or physician associate(PA) is a health care practitioner who practices medicine in collaboration with or under the (indirect) supervision of a physician, depending on state laws (equivalent to a nurse practitioner). Physicians do not need to be on-site with PAs and collaboration or supervision often occurs via electronic means when consults are necessary. Their scope of practice varies by jurisdiction and healthcare setting. In the United States, PAs are nationally certified and state licensed to practice medicine at their level. PAs in the U.S. are trained with the “medical model” and complete the qualifications for their certification in considerably less time than a traditional medical degree by following an educational model based on the fast-tracked training of physicians during World War II. In the United Kingdom there has been an expansion of the PA workforce, and regulation under the General Medical Council was announced in 2019.
In the United States, PAs are nationally certified and state licensed to practice medicine at their level. PAs in the U.S. are trained with the “medical model” and complete the qualifications for their certification in considerably less time than a traditional medical degree by following an educational model based on the fast-tracked training of physicians during World War II. In the United Kingdom there has been an expansion of the PA workforce, and regulation under the General Medical Council was announced in 2019. We are clinical officers but different names.
We are clinical officers but different names.
Author: SITE LIVE
BREASTFEEDING GUIDELINE
Breastfeeding is the most natural way to feed your baby. It provides all the nutrition your baby needs during the first six months of life, satisfies their hunger and thirst at the same time. It also helps to create a loving bond between you and your baby.

Breast milk has a number of health benefits for your baby:
- breastmilk contains all the nutrients your baby needs for the first 6 months
- it also satisfies the baby’s thirst
- it helps develop the eyes and brain and other body systems
- the act of breastfeeding helps with jaw development
- it helps the baby resist infection and disease, even later in life
- it reduces the risk of obesity in childhood and later in life
- it contains a range of factors that protect your baby while their immune system is still developing
Breastfeeding also has many benefits for mothers. Not only is it convenient, cheap, and always available, it also:
- reduces the risk of haemorrhage immediately after delivery
- reduces your risk of breast and ovarian cancer
- is convenient and cheap
- can soothe your baby
- prolongs the amount of time before you get your period again
Getting started
You can usually start breastfeeding within the first hour or so of your baby’s birth.
The first milk in your breasts is called colostrum. This milk is quite thick and may be yellowish in colour. It’s very rich in protein and antibodies that will help give your baby a great start in life. Mature breast milk gradually replaces the colostrum in the first few days after birth.
Ideally, you should try to maintain close skin-to-skin contact with your baby immediately after the delivery. If you hold your baby against your chest and between your breasts for a while, there’s a good chance he or she will find your nipple and begin feeding without any help. Your midwife or a lactation consultant can also help guide you and your baby into position.
Good positioning and attachment
The key to successful breastfeeding is comfortable positioning and good attachment.
If your baby is well-attached to your breast you are less likely to experience breastfeeding problems like cracked nipples, and your baby will get the most amount of milk out of your breast.
There are lots of different ways to position and attach your baby for breastfeeding, but here are some general tips:
- Sit comfortably with your back and feet supported – you can be fully upright or you might prefer to be laying back a little bit.
- Unwrap your baby and hold him or her close against you.
- Turn your baby on his or her side so they are wrapped around you with their nose level with your nipple.
- Make sure you support your baby’s neck and shoulders with your hand, but don’t hold your baby’s head — allow him or her to find the best position for attaching to your breast.
- Bring your baby to your breast, not your breast to your baby.
- Gently brush your baby’s mouth with the underside of your areola (the area around the nipple) — this will usually cause your baby to open their mouth very wide.
- When your baby opens their mouth, bring him or her quickly to your breast so they take a good mouthful of breast tissue.
- As you bring your baby to your breast it can help to hold your breast like you would a sandwich, with your nipple aimed at the roof of your baby’s mouth.
Signs that your baby is well-attached include:
- Your baby’s chin should be tucked into your breast, and his or her mouth should be wide open with the bottom lip curled back.
- Your baby’s nose will be clear or only just be touching your breast.
- More of your areola will be visible above your baby’s top lip than below it.
- Your baby’s cheeks should not be sucking in and there should be no clicking noise during sucking.
- There should be no nipple pain — but you might feel a stretching sensation as your nipple adjusts to breastfeeding.
How often will my baby feed?
During the first week of life most babies will gradually develop a pattern of feeding eight to twelve times in a 24-hour period. You should feed your baby whenever he or she shows signs of hunger.
You will know your baby is getting enough breast milk if he or she:
- is feeding at least 8 times a day (with some of those feeds occurring overnight)
- has at least 5 wet disposable nappies or 6 to 8 wet cloth nappies per day
- has 2 or more soft or runny bowel movements per day for around the first 6 weeks of life (babies have fewer bowel movements once they reach about 6 weeks)
- is gaining weight and growing as expected
- is alert when awake, and reasonably contented
Building your milk supply
When it comes to breastfeeding, supply equals demand. The more you feed your baby, the more milk your breasts will make. Some tips for establishing and maintaining a good milk supply include:
- let your baby feed until he or she stops sucking and swallowing and lets go of your breast, and then offer your second breast
- offer your breast at night as well as during the day
- avoid giving any extra feeds from bottles, as this reduces your baby’s need to suck at your breast and reduces your milk supply
- avoid the use of dummies (pacifiers)
Managing problems
Breastfeeding is natural, but it’s also a learning process for you and your baby. Sometimes problems develop. Don’t be afraid to ask for help at any stage during your breastfeeding journey.
Hard-to-tell DIFFERENCE FOR MOST KENYANS WHO HAVE BEEN ATTENDED TO BY THE HANDS OF MEDICAL OFFICERS OR CLINICAL OFFICERS.
A white dustcoat, a stethoscope dangling around the neck, a writing pad on the table and a pen in hand.
Clinical officers site live question is Are you being attended to by a doctor or a clinical officer?
This is often a hard-to-tell difference for most Kenyans who have been attended to by the meticulous hands of clinical officers.
Doctors and clinical officers in a health institution show similar medicine technical know-how and professional skills.
Clinical officers are health professionals train in diploma comprising clinical medicine and surgery for three years and one year mandatory internship, upon which they are registered and licensed under the Clinical Officers Council, which is also their professional regulatory body.
MEDICINE
Clinical officers are registered in accordance to a law reviewed on June 2017.
There are about 20,000 registered clinical officers in the country.
Of these, 7,757 clinical officers are working under the national and county governments while another estimated 600 work on government capacity building programmes in NGOs.
A higher level of clinical officer undergoes clinical medicine for five years and one year of internship.
PERSONNEL
With this, they can perform caesarean section and minimal intrusive surgery, such as circumcisions.
They are also qualified to offer orthopedic services.
The higher diploma cadre of clinical officers creates a pool of specialised health officials.
They work as consultants in fields such as oncology, paediatrics, dermatology, ophthalmology, anaesthesia, obstetrics and gynaecology, nephrology.
They also render services in chronic illness and management such as diabetes and hypertension.
Proud: Clinical Officer
The Clinical Officers Council (COC) is mandated to train, register and license clinical officers working in Kenya.

CLINICAL OFFICERS COUNCIL Registration
The Council registers all students trained in approved training institutions and assess students trained out of the country as well as national trained students. The Council approves all the training institution to ensure quality training.
The Council administers registration exams to ensure competency of all registered clinical officers.
Required Documents for Registration
Identification Card
Degree/Diploma Certificate
KCSE certificate
Internship completion letter
Internship Booklet/Logbook
Recently taken passport size photo
Registration Fees
1. Diploma – ksh 7000
2. Degree – ksh 7500
3. CPD diary fees – ksh 500
4. Code of conduct- ksh 500
N/B The above fees are not permanent, are subject to change under sole discretion of Clinical Officers Council
Clinical Officers Licensing
The council gives a practicing license to qualified clinical officers in both public and private sector .
The practicing license is renewed after two (2) years, but clinical officers in private practice renew the licenses annually.
Clinical Officers Council Licensing Renewal Charges
The practicing Clinical officers renewal charges are : ksh 2500 payable via :
1. M-pesa Paybill no: 325100 , A/c no : Student registration number
2. Cooperative Bank Branch: NBC , A/c no: 01102039922700 , A/c name: Clinical Officers Council.
N/B The fees above are subject to Change under the sole discretion of COC
Clinical Officers Council Office location, directions and Contacts
The Clinical officers Council offices are located at Blue Violet Building, suite 203 , Kindaruma road ,off Ngong Road Nairobi.
Phone: +254 725 705 144
Email: info@clinicalofficerscouncil.org
Huge pay gaps in counties as SRC sits on report

CLINICAL OFFICER EARNS ABOUT Sh74,830 PER MONTH
On 2nd February 2019 Doctors issue strike notice over SCR job review
DETAILS have emerged of glaring salary disparities among counties’ staff, even as the Salaries and Remuneration Committee sits on a report that could go a long way to bridge the gaps.
The Star has established various cadres — especially in the health sector — are worlds apart in terms of pay, despite similar academic qualifications.
Human resource experts warn the huge salary and allowance gaps could fuel strikes as workers push for enhanced pay.
Pay structures obtained by the Star from select health sector workers reveal details of the pay discrepancies, with certain staff cadres earning twice the monthly gross salary of their colleagues.
Staff with diploma qualifications, regardless of the sector, join the service at job group H but their salaries and allowances differ significantly.
For instance, a nurse joining with a diploma starts with a basic salary of Sh23,780, while a civil, mechanical or electrical technician earns Sh24,380 monthly basic salary.
The nurses also pocket a Sh10,000 annual uniform allowance. They are currently agitating for that allowance to be increased to Sh25,000, as negotiated in their CBA in 2017.
However, while the engineers at diploma level pocket a Sh3,200 housing allowance and Sh4,000 commuter allowance, the nurses receive an array of enhanced allowances.
Veterinary officers with diploma qualifications earn a basic salary of Sh24,000 and Sh3,200 and Sh4,000 as house and commuter allowances, respectively. The gross monthly pay for veterinary, electrical, mechanical and civil technicians is Sh31,000.
Nurses and clinical officers receive other allowances over and above what their counterparts earn.
They are entitled to Sh20,000 extraneous allowance, Sh20,000 practicing allowance and Sh3,850 risk allowance. They also get commuter allowance of Sh4,000 and house allowance of Sh3,200.
This means that a diploma holder nurse or clinical officer earns about Sh74,830 per month, more than twice what their technician colleagues take home.
A graduate engineer and architect earns a monthly basic salary of Sh35,260, a housing allowance of Sh7,500 and a commuter allowance of Sh5,000.
This brings their monthly gross pay to Sh47,760, a far cry from what nurses and clinical officers take home.
Further compounding the pay disparities, a laboratory technician holding a diploma enters the service at job group H with a starting pay of Sh23,780.
They are entitled to a house allowance of Sh3,200, commuter allowance of Sh4,000 and risk allowance of Sh3,850.
If the 2017 Collective Bargain Agreement between the Kenya Union of Nurses and the counties is implemented, the nursing allowance will increase to Sh30,000, up from Sh20,000 and the uniform allowance will be pegged at Sh25,000 a month.
Tabulations by the SRC show that the nursing allowance alone will cost counties Sh2.9 billion and the national government Sh146 million to implement the CBA.
The uniform allowance ill cost counties Sh365 million, while the state will spend Sh383 million.
Apart from medical officer, specialists, and dentists, the other cadre of health officers includes nurses, clinical officers, dental technologists, oral health workers, public health technicians, pharmacy technologists, laboratory technologists, orthopaedic technologists, nutritionists, radiologists and physiotherapists.
Others are occupational therapists, health record technicians, plaster technicians, medical engineers and engineering technicians and community health workers.
Despite the blatant pay disparities, the Salaries and Remuneration Commission that conducted a job evaluation to harmonise the salaries and allowances is delaying on its final report.
The SRC, mandated to set and review salaries and benefits of all civil servants, was expected to release the report a few weeks ago but it was shelved under unclear circumstances.
The report is considered key in addressing pay disparities among county staff following the latest nurses’ strike. It is feared a ripple-effect could paralyse the counties.
The Labour and Industrial Court suspended the nurses strike for 60 days, pending conciliatory efforts between the nurses’ union and labour experts appointed by Labour CS Ukur Yattani.
The Star is informed the SRC held a stormy crisis meeting with the Council of Governors on Tuesday. It was meant to discuss the withheld report, which recommends sweeping changes.
That meeting informed the SRC’s decision to ask counties not to strike any pay increment deals without SRC input.
The SRC warned that unstructured awards of salary and other allowances is not sustainable and could lead to disharmony and a spiralling across the sector.
“As a result of the continuous clamour for enhancement of allowances, nurses are currently remunerated higher than comparable grades within the public service,” the SRC said in a statement.
Read:
“Consequently, payment of the above allowances will result in inequity in terms of remuneration for comparable jobs in the health sector and in the entire public service. This may give rise to demands for harmonisation within the health sector and possibly the entire public service, further pushing up the public wage bill,” the SRC said.
During Tuesday’ meeting, the SRC is said to have accused some governors of entering into binding pay deals with employees without involving it, in what it said could soon spark a nationwide spreading of demands.
It is said the SRC was categorically against any pay hikes, considering ongoing salary harmonisation as well as the country’s ballooning wage bill of more than Sh600 billion annually.
An SRC commissioner, speaking on condition of anonymity, said some of the allowances for staff working at the counties were illegal.
“This is what we are grappling with as a commission. We are concerned counties introduced irregular allowances especially for nurses for political reasons,” he said.
He warned, “What is happening in the health sector is messy. There is political games going on that could impact negatively on job evaluation. Counties must know that when they give in to nurses they should prepare for a ripple effect from other cadres of employees.”
Yesterday CoG chairman Wycliffe Oparanya protested against delay in releasing the job evaluation report by the SRC, saying failure to conclude the document in time has triggered pay increase demands among county workers.
“The SRC has been dillydallying with this report. It is important that it is realised so salaries are harmonised across all county employees,” Oparanya said.
“All county staff must have all salaries and allowances harmonised with other employees, according to the SRC requirements. As counties we don’t set salaries and benefits for our employees. That’s the SRC’s work,” he said.
Chairman for the Kenya Union of Clinical Officers Peterson Wachira yesterday admitted there are glaring pay disparities at the counties, saying his union would call a strike if CBA negotiations don’t not resume.
“It is true there are disparities. Some staff inherited from local authorities earn more than those who joined county governments. There are huge discrepancies in the allowances that must be addressed,” he told the Star.
Fears of a ripple effect have gripped the counties after clinical officers issued a 14-day strike notice if CBA talks stall.
NEWS:CLINICAL OFFIERS SITE LIVE
TIPS FOR USING PEP EFFECTIVELY Think you might have put yourself risk? Read on about PEP.

You’ve just had a hot night, but weren’t as safe as you could have been, and now you’re thinking about the possibility that you might have been exposed to HIV. If so, PEP may be your answer.
Post-Exposure Prophylaxis ( PEP) is a four week course of anti-HIV medications taken daily (in pill form) that can potentially stop HIV infection after exposure. PEP must be started within 72 hours of exposure though the sooner you start taking it the better.
1. Know when to use it
You should consider getting PEP to stop HIV as soon as possible if you have:
Had a condom break during anal sex
Had anal sex with no condom in particular if you’re were bottoming and your partner ejaculated in your arse, or
Shared syringes for injecting any substance
In any case call the 24/7 PEP hotline: 1800 PEP NOW ( 1800 737 669 ) as soon as you think you’ve been exposed to HIV.
2. Know when NOT to use it
PEP is not recommended after oral sex or other low risk activities. If you’re not sure how risky it might have been, make sure you
know the risk and talk to a healthcare professional or call the PEP hotline. Though it might not be a risk for HIV, you could still pick up other STIs which is why it’s important that all sexually active gay men test often; at least twice a year and more if you have a lot of partners.
3. Give yourself the best chance of it working
To be most effective, PEP should be started within a few hours of exposure to HIV. If it is not started within 72 hours (3 days) it is not likely to work. So the sooner it’s started after exposure, the greater the chance of working.
Make sure you complete the full course of treatment as well to give yourself the best odds against infection: take your medication every day for one month without missing a dose and do not stop taking your prescribed doses without talking to your doctor.
4. Understand the potential side effects
As with most antiretroviral drugs, PEP can cause side effects such as diarrhoea, headaches, nausea/vomiting and fatigue. However these are usually mild and generally only last a few days with no long-term side effects. Speak with your GP or sexual health clinic if you have any concerns.
5. Plan for the future
There is no guarantee that PEP will prevent infection. In any case, we recommend you to continue to stay safe.
There are now at least five strategies that ACON defines as ‘safe sex’, provided that certain parameters are met. They are:
1. The use of condoms for casual encounters
2. PrEP: HIV negative men taking pre-exposure prophylaxis (PrEP) every day. PrEP is currently not approved by the Therapeutic Goods Administration (TGA). Click here to find out options to access PrEP in Australia
3. UVL: Men living with HIV who have a sustained undetectable viral load (UVL) and no sexually transmissible infections (STIs) for at least six months
4. Use of serosorting between HIV positive men, and
5. Negotiated safety agreements, where both partners have established their sero-status and have had no risk incidents
If you think you may have been exposed to HIV you should consider getting PEP now. Contact your local sexual health clinic, hospital accident and emergency department
Guidelines : clinical officers site live
OTHER NAMES OF CLINICAL OFFICER
1)Osteopathic physicians , Podiatrists ,
Optometrists and Anesthesiologist assistants in the United States
2)Emergency and Clinical Officer Pakistan
3)Physician Assistants in the United States, United Kingdom, Netherlands, Liberia and
Ghana
4)Assistant Doctors in China,
5)Surgical Care and Emergency 6)Care Practitioners in the UK,
7)Assistant Physicians in Saudi Arabia,
8)Health Extension Officers in Papua New Guinea
9)medical assistants/Sub Assistant Community Medical Officer in Bangladesh
10)Medical Assistants in Fiji
11)Assistant Medical Officers in Malaysia
12)Surgical Technologists in Mozambique
13)Clinical Associates in South Africa.
14)Clinical officers in East Africa, Central Africa, West Africa and other parts of Africa
A
MEDICAL OFFICERS AND CLINICAL OFFICERS TRAINING DIFFERENCE AND SIMMILARITIES

MEDICAL OFFICERS TRAINING:
1)Is a six-year professional degree programme accredited by the Medical Practitioners and Dentists Board involving
2)Two years of pre-clinical training in medical sciences followed by
Four years of training in clinical medicine, surgery and community health including a mandatory one year internship and
Registration, licensing and gazettment by the Medical Practitioners and Dentists Board giving
Unlimited practice rights with
Specialisation and private practice allowed and eligible for full professional membership of the Kenya Medical Association (KMA)
CLINICAL OFFICERS TRAINING:
1)Is a four or five-year professional diploma or degree programme accredited by the Clinical Officers Council involving
2)One year of pre-clinical training in medical sciences followed by
Three or four years of training in clinical medicine, surgery and community health including a mandatory one year internship and
Registration, licensing and gazettment by the Clinical Officers Council giving
Unlimited practice rights with
Specialisation and private practice allowed and eligible for full professional membership of the Kenya Clinical Officers Association (KCOA)
The current training follows international guidelines and the two qualifications are awarded jointly on successful completion of a comprehensive nine trimester programme of full-time study, practicals and examinations which are covered over three years leading to a fourth mandatory year of internship in a teaching hospital. A fifth and sixth residency specialisation years are undertaken after registration by the Clinical Officers Council and three years of work experience in general medicine which leads to the award of a general degree in clinical medicine or a specialist
diploma in pediatrics, orthopedics , psychiatry ,
anaesthesia, reproductive health and other specialties.
A clinical officer is therefore able to graduate and join the workforce in a minimum of four calendar years and provides medical services within the full scope of family and emergency medicine or within a narrower scope depending on their area of specialisation.
Registration by the Clinical Officers Council (COC) entitles one to render medical services in any public or private medical institution or to practice medicine independently as a private practitioner. Registration also qualifies one to join and participate in the affairs of the Kenya Clinical Officers Association (KCOA) , including its annual KCOA Scientific Conference , and the
Kenya Union of Clinical Officers (KUCO) . As per the government’s Revised Scheme of Service for Clinical Personnel (2014) a clinical officer works at any of 8 grades depending on ones seniority.
As gazetted officers all registered clinical officers are legally authorized to prepare, sign, issue and keep safe custody of official state documents such as medical examination reports, sick notes , postmortem examination reports and death certificates and to appear in courts of law as expert witnesses. For this reason, a clinical officer is the officer in-charge of a health center or a district hospital and is part of the medical team in bigger hospitals where one may head a department or work under a senior clinical officer or a physician.
Clinical officers are direct healthcare providers who manage and administer health institutions, medical schemes and projects in primary healthcare (PHC) settings and are frontline stakeholders in Universal Health Coverage in
Kenya which is one of the key pillars of the government’s 5-year development plan under
President Uhuru Kenyatta . The four pillars of the 5-year development plan are
1.Manufacturing
2. Affordable housing
3.Universal Health Coverage
4. Food security .
HIV Infection in 2019: A Cure Is Not the Real News
The announcement of the London patient , the second person cured of HIV infection through hematopoietic stem cell transplant, sent waves through the media and spurred a series of inaccurate headlines that put HIV back into focus for people who do not think about it often. We Clinical Officers Site Live received a series of text messages along the lines of “Did you hear about the HIV cure?” and “we heard there’s someone in Europe with a cure for AIDS.” Because these came from intelligent, nonmedical people, it led us to reflect on the paucity of knowledge that most people have about the breakthroughs in HIV management and therapies.

One-pill regimens have been a reality for HIV regimens since the approval of efavirenz, emtricitabine, and tenofovir disoproxil fumarate (Atripla) more than 10 years ago. This revolution has continued with integrase strand transfer inhibitor (INSTI)–based regimens earlier this decade. Regimens containing 3 drugs can be replaced with 2-drug regimens, sparing patients from exposure to a third agent. In many ways, therapy for HIV infection has become easier to manage than that of diabetes. However, this is not well known outside infectious diseases clinicians, and even many HIV care practitioners are hesitant to transition patients whose infection is undetectable on an older 3-drug regimen to a novel regimen that decreases antiretroviral exposure.

Pre-exposure prophylaxis (PrEP) has transformed HIV prevention. Patients at high risk who are taking a single, well-tolerated antiretroviral are well protected from HIV infection, as is the public, by a reduction in transmission. It is a true public health revolution. However, the benefit has reached communities that are at risk at varying levels. Coastal gateway cities that formerly had the highest incidence of HIV infection but have instituted PrEP programs have been replaced by cities in the Southeast. Cities with a high prevalence and that provide PrEP programs are seeing the incidence drop. Despite high coverage by insurance companies, only a small proportion of patients who could benefit from PrEP currently receive it. Much needs to be done to spread the word to primary care providers and other clinicians, including pharmacists, nurse practitioners, and physician’s assistants (Clinical officers) to screen and recommend PrEP when appropriate.
Finally, the U=U (undetectable=untransmittable) campaign has given a catchy title to an important principle but one that is not well known enough.

It will take time to break down the stigma of HIV infection that has built up over decades, but overcoming that barrier is vitally important for the physical and mental health of millions of people. Using treatment as prevention may not be as catchy as “finding a cure” for HIV, but it is certainly much more realistic. Implementing this treatment will become only easier as new long-acting maintenance injectable antiretrovirals become available in the near future.

These areas of HIV medicine have in common a lack of sufficient awareness. Each is a major step forward from early therapies, advancing HIV from a death sentence to a chronic condition to the next step, which is making it an uncommon chronic condition in the United States and carrying advances forward into other countries. We may not have a cure, but we sure have come a long way. Let’s make certain that everyone knows it.
On the topic of HIV, this issue of Clinical Officers Site Live features a review of a new INSTI combination, an article on event-driven PrEP; and highlights from the Annual Conference on Retroviruses and Opportunistic Infections . Our feature article this month, “ Four Fungal Horsemen: Emerging Trends in Fungal Disease Epidemiology,” discusses several emerging fungal infections that may appear in unexpected places.
As always, enjoy this issue, and keep up with us at Clinical Officers Site Live .
Leave a comment
ANAESTHETISTS CLINICAL OFFICERS are the highest earning professionals in CLINICAL OFFICERS SPECIALIZATIONS
A career in anaesthesia is the most lucrative and best paying clinical officers specialization in Kenya.
Anaesthetists are health-care providers who specialise in drugs and processes that patients require before, during and after surgery.
This ensures patients are comfortable during surgery.
As an anaesthetist, one monitors patients closely after surgery to make sure they recover comfortably. With devolution, opportunities for anaesthetists exists in county government referral hospitals.
In 2016, patients at Nyeri Referral Hospital had to wait for long due to a shortage of anaesthetists. The hospital requires 15 anaesthetists for theatres to operate optimally; four to work at night and two during the day shift, two on call and an additional eight to relieve their colleagues. However, the hospital had only five specialists by the time of the incident.
Infant mortality.
The problem is the same in other counties. In Wajir County, for the past 50 years, the county’s Habasweni District Hospital in Wajir South Constituency has not had the services of anaesthetists.
When the international community discusses how to address Millennium Development Goals four and five, increasing maternal health and reducing infant mortality, lack of access to properly administered anaesthesia is rarely part of the conversation.
In Sub-Saharan Africa, the shortage of anaesthesia providers to assist during deliveries has exacerbated the issue of maternal and infant mortality.
Improperly administered anaesthesia, or complete lack of anaesthesia, is one of the top four causes of death in rural hospitals among maternal patients during labour in Sub-Saharan Africa.
The World Journal of Surgery reported in 2010 that only 13 of approximately 120 anaesthesiologists in Kenya work in public hospitals. The remainder are in private practice in Nairobi, with few working in the rural areas. It is estimated that in rural areas, there is only one anaesthesiologist for every 13 surgeons.
In 2016 Phoebe Khagame, Administrator at Kenya Society of Anaesthesiologists (KSA) via the standard news paper stipulated that , there’s a huge deficit, as the numbers available are far below the recommended WHO anaesthesia to patient ratio.
“We currently have about 150 physician anaesthesiologists, of whom about 50 are in public service with the rest in private practice, and about 60 registrars in training,” says Khagame.
So,what does it take for one to study the course and in which universities is the course offered? Anaesthesia services in Kenya are provided by three cadres of practitioners.
Physician anaesthesiologists are medical doctors who first train as medical officers for six years. After registration as medical officers, they study for four years for a Master of Medicine in Anaesthesia, offered by University of Nairobi and Aga Khan University Hospital.
Registered Clinical Officers Anaesthetists (RCOs) are diploma graduates in clinical medicine from Kenya Medical Training College (KMTC), who can pursue Higher Diploma in Anaesthesia for 18 months at Kenya Medical Training centres, such as Nakuru, Nairobi and Kisumu.
Finally, are Kenya registered nurse Anaesthetists (KRNA), who are also diploma graduates in nursing. They can also pursue a higher diploma in Anaesthesia. There are currently two training institutions, Kijabe Hospital and Kisumu KMTC.
Remuneration is not commensurate with the workload, which sometimes results in practitioners moving to private practice, as that pays better.
“The work of anaesthesia providers has for a long time been misunderstood by other health professionals and the public in general and hence it hasn’t been publicised properly,” says Dr Susan Nabulindo.
The practitioners can also provide emergency services in organisations like Red Cross and AMREF, where they are involved in transfer of patients. Anaesthesiologists are also involved in training, education and leadership roles in institutions where they work.
PROUD CLINICAL OFFICERS
SHARE AND COMMENT
